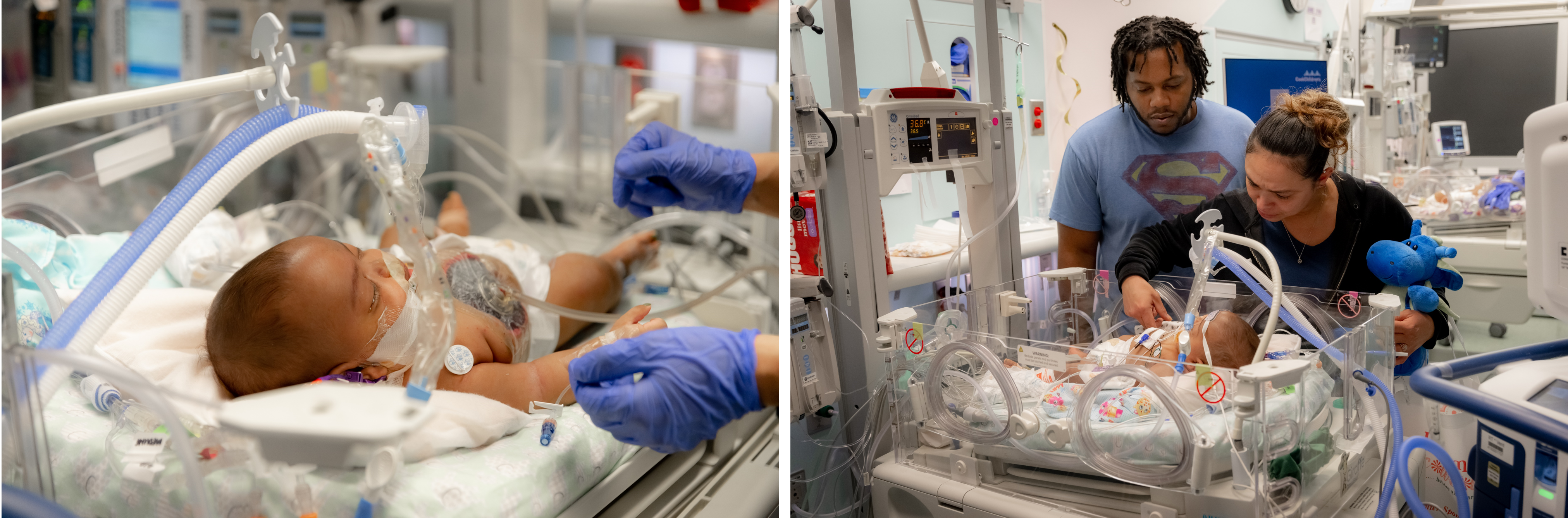
The phrase “joined at the hip” has taken on a new meaning for AmieLynn Rose and JamieLynn Rae Finley, who were born Oct. 3, 2022, literally joined from their chest to their belly buttons. The conjoined twins, who shared a liver, were born at 34 weeks gestation, weighing a combined 4 kilos (8.82 pounds).
The connected sisters would embark upon a long journey in the neonatal intensive care units (NICUs) at two renowned Fort Worth, Texas, hospitals leading up to their separation when they were almost four months old.
The Shock of a Lifetime
Amie and Jamie’s parents, Amanda Arciniega and James Finley, were stunned to learn they were expecting conjoined twins during a 10-week routine ultrasound with Amanda’s obstetrician.
Shortly after, the couple was sent to maternal-fetal medicine specialist Bannie Lee Tabor, M.D., with Maternal-Fetal Medicine of Texas, part of Pediatrix® Medical Group.
Specializing in high-risk, complex pregnancies, Dr. Tabor managed Amanda’s prenatal care and monitored the babies’ development and well-being throughout her pregnancy. When it was time for the twins to be delivered, he performed a Cesarean section at Texas Health Harris Methodist Hospital Fort Worth.
“Typically, we’ll go to 37 weeks gestation with non-conjoined twins,” said Dr. Tabor. “With this case, the need to deliver at 34 weeks was becoming a mechanical issue. Their growth was dropping off a bit, so it was time to get them out. Additionally, the need to do so while minimizing the amount of trauma to the babies and the mom was essential.”
Delivery was a success, and the twin girls spent their first six weeks in the hospital’s NICU before being transferred to the NICU at Cook Children’s Medical Center Fort Worth. Fortunately, Pediatrix neonatologists Mary Frances Lynch, M.D., and Chad Barber, M.D., care for babies at both hospitals, allowing them to provide seamless, ongoing care to Amie and Jamie.
“The same doctors and neonatal nurse practitioners are at both hospitals. At each hospital, certain nurses signed up to provide primary nursing care for these babies throughout their NICU stay,” said Dr. Lynch. “These primary nurses have gotten to know the family, and they know the babies and their quirks and the things they like and dislike. Delivering the type of individualized care they do really makes a big difference for a family that can’t take their babies home just yet.”
Dr. Barber agreed that the role of neonatal nurse practitioners and primary nurses is instrumental as the babies grow and develop.
“Especially during the month and a half prior to separation, the role the advanced practitioners and primary nurses played was even bigger because the babies were getting older and clinicians had to start working on the babies’ developmental growth,” he said. “Their job responsibilities increased greatly because it’s not just feeding and changing diapers and providing other care. They had to play with them and make sure the babies were hitting all the developmental milestones of a normal two-month-old, as best they could while still being attached as a single unit. It would have been impossible without the neonatal nurses and nurse practitioners.”
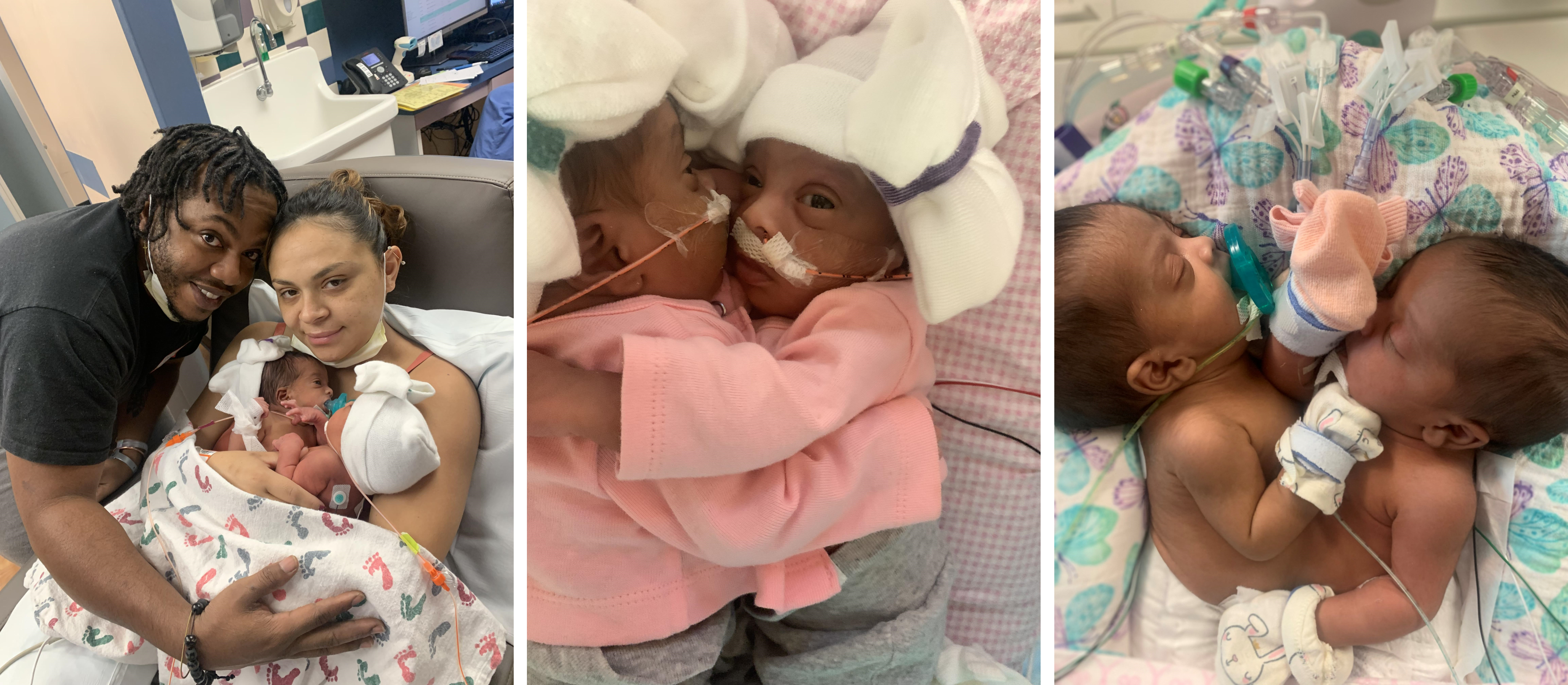
Two Babies, One Bed
Caring for conjoined twins in the NICU is similar to caring for single babies. Still, there are vast differences and unique challenges.
“In some ways, things are very much the same, and in other ways, it is very different because there are aspects we don’t typically have to think about with single babies, positioning being a big one,” said Dr. Barber. “Holding conjoined twins is not easy. Feeding is not easy, especially when you have to feed one at a time because they are facing each other. We always had to make sure they were in a good position.”
In addition, tasks like changing diapers and clothes, bathing and providing medical care aren’t as challenging with singletons as they are with conjoined twins. For the most part, Amie and Jamie had completely separate bodies, but they shared a large liver. Therefore, they shared blood circulation, which came into play when giving medicines.
“We had to think a little harder about medication and immunization administration and how to dose the babies,” said Dr. Lynch. “We had to determine if we should treat them as one baby and give them a larger dose than a single baby weighing the same would receive or if we should give each baby a dose of medicine based on their estimated individual weights. It came down to doing our best to figure out how much shared blood flow they had and making our best estimate. We learned they shared a significant amount of blood when we gave one baby a blood transfusion and both babies’ red blood cell counts went up.”
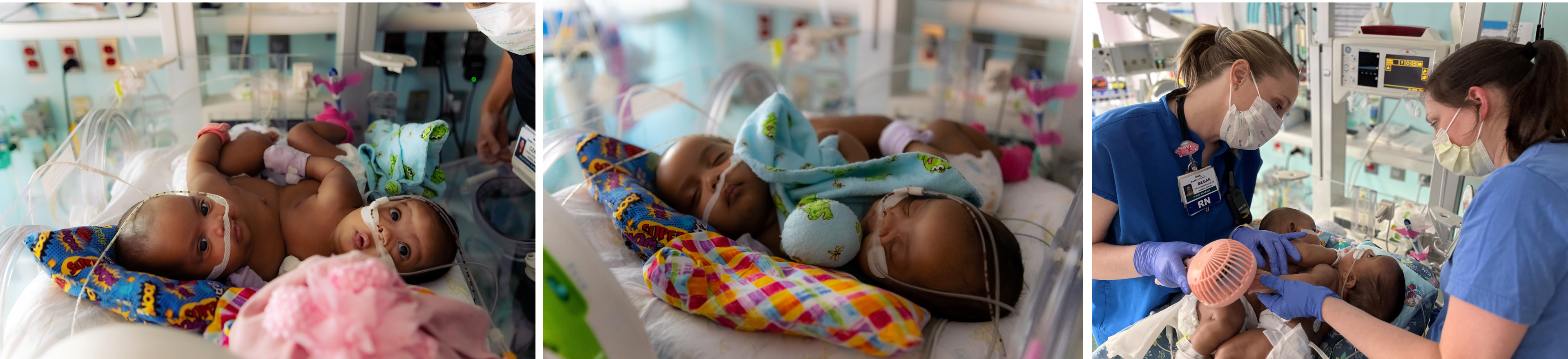
Separation Day
Jan. 23 was an emotional, much-anticipated day for parents Amanda and James and a team of more than 25 medical professionals. An 11-hour surgery would separate Amie and Jamie, the first of its kind at 105-year-old Cook Children’s Medical Center.
Because there would be so many adults in a small space, simulation was a critical aspect of the months-long preparation. Simulation exercises before delivery and before separation helped ensure every medical professional knew his or her role with great precision.
“Before delivery, simulating was essential so that if one of the babies needed breathing support, for example, we knew exactly who was going to do it and where they would stand at the bedside,” said Dr. Lynch. “If one would need to be intubated, we practiced that process to help ensure the stability of the other twin. We went through a lot of different scenarios and made sure we had a ton of extra equipment for all the ‘just-in-case things,’ so if it happened in the moment, we knew how we would approach them.”
The highly complex surgery required two teams — one for each baby — and hours of practice drills. In addition, each baby and her corresponding team were color-coordinated. One baby’s assigned color was purple, and her team wore purple hats, while the other’s color was green.
“Putting the entire team through countless simulations really prepared us leading up to the separation so on the day of the surgery, we were prepared for any and all scenarios,” said Dr. Barber. “It was somewhat easier because we had already done this for their birth, so we already had the colors picked out and followed similar procedures.”
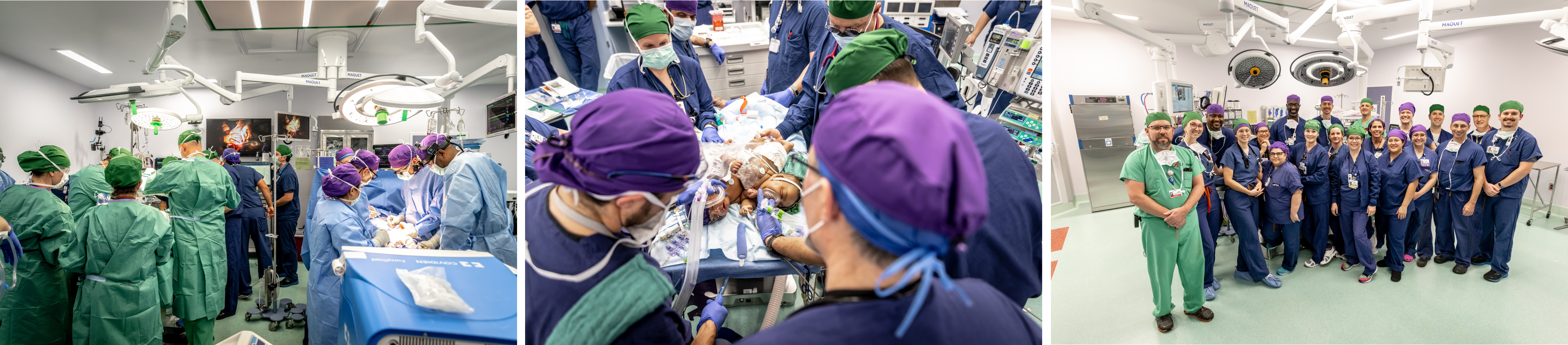
After an 11-hour wait, Amanda and James were given the news that their daughters had been successfully separated.
“They came back to me,” James said during a news conference after the separation. “I told them to come back to me, and they did.”
While the separation was a huge milestone, the girls’ recoveries will take an undetermined amount of time. They still have a long way to go.
Two Babies’ Road to Recovery
Separating conjoined twins is an extremely complex surgery, and recovery doesn’t happen overnight. While Amie and Jamie are doing well overall, there will be challenges along the way.
“In some ways, their early recovery has been smoother than expected,” said Dr. Lynch. “They were a lot more physically stable than I had anticipated. The biggest issues are pain control and sedation, which have been way more challenging than we had expected.”
Aside from the medical aspect of their recovery, Amie and Jamie face adjusting to their new lives as separate individuals on several levels: physically, emotionally and developmentally.
“They really are not OK with being separated because they’ve always been connected,” said Dr. Lynch. “Before surgery, they had not needed much respiratory help, and they hadn’t been hooked up to a lot of wires and lines. So, to suddenly have a ventilator and all these IVs was probably really scary for them. That was a challenge that was a little more pronounced than I had expected.”
The journey has also been very scary for their parents. During the news conference, James described their experience leading up to the surgery.
“It was like walking through a haunted house,” he said. “You just got to get through it. It’s scary, very scary and emotional, but you just got to keep going and get through it.”
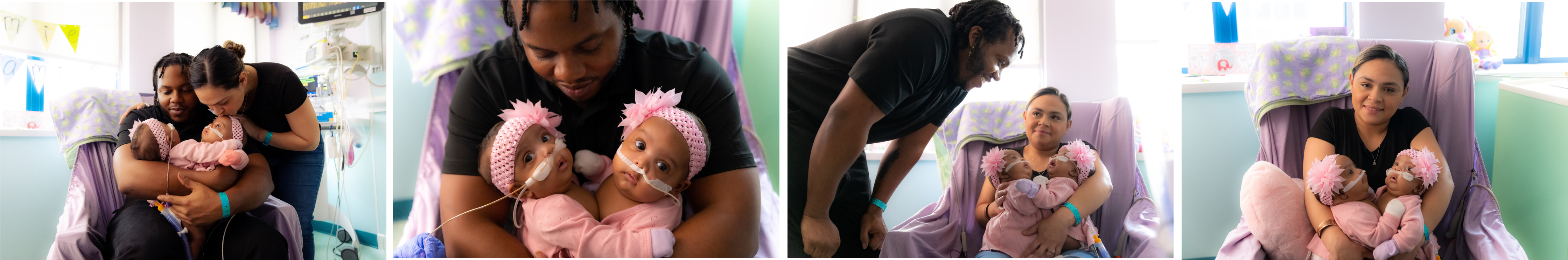
Holding Two Babies for the First Time
It was an exciting, emotional time when Amanda and James got to hold Amie and Jamie for the first time as two separate babies. It was equally emotional for many of the medical professionals who have cared for the twins as their own.
“It was pretty emotional for everyone,” said Dr. Barber. “I think the nurses were just as emotional as mom and dad.”
The nurses at the bedside are with the babies more than anyone. The care they provide is every bit as vital to the twins’ recovery as it was pre-surgery.
“The nursing staff makes all the difference,” said Dr. Lynch. “They are at the bedside with them for 12 hours at a time, providing all the care, making sure they are developing appropriately, making sure their diapers are changed and they’re not getting diaper rash, ensuring they are fed when they need to be and that they are getting consoled, loved and held and all those vital things. It doesn’t happen without the attentiveness of the nurses.”
It’s been five weeks since the girls’ separation, and the NICU team’s unwavering dedication to their care and well-being remains steady.
“We really love your girls and have put our hearts and souls into them and will continue to do so as long as they need us,” Dr. Lynch told Amanda and James during a Fort Worth news conference.