A newborn hearing screen, performed shortly after birth, is essential to help identify babies at risk for hearing loss. Hospitals either use their own staff to perform screens or partner with a third-party provider, such as Pediatrix Newborn Hearing Screen Program, a MEDNAX affiliate. Because there is so much activity that occurs in the hospital after your baby is born, you may not even know the screen has been performed.
In recognition of Better Hearing & Speech Month, we encourage all expecting and new parents to educate themselves about the importance of hearing health. Roughly 2 to 3 infants out of every 1,000 births will experience hearing loss. Hearing loss may occur in one or both ears, it may be to varying degrees, it may change over time and it may come without factors such as a family history. Experts agree it is important to diagnosis and treat hearing loss early. This can help avoid delays in childhood speech, language, social and academic skills. To learn more, here are some questions you can ask of your hearing screen provider before your baby is screened.
How much experience do you have?
Practical newborn hearing screen experience matters. Experience and quality go hand-in-hand. A quality program minimizes inaccurate results, which you may hear as "false negatives" or "false positives." For a baby who does not pass a hearing screen, the infant's result will recommend referral for follow-up testing. Your screener will probably say, "Your baby has referred the hearing screen."
It is important that hearing screens correctly identify babies at risk for potential hearing loss. If a baby incorrectly passes a screen, the baby may not be referred for audiology follow-up. If a baby incorrectly refers a hearing screen, this could lead to stress for parents and unnecessary use of often scarce community resources.
The Pediatrix Newborn Hearing Screen Program has more than 20 years of experience. Annually, Pediatrix screens 800,000 babies in more than 30 states, providing services to over 400 hospitals. The American Academy of Pediatrics advocates for a screening program’s referral rate—meaning the number of infants referred for additional hearing assessment by an audiology professional—not to exceed 4 percent; our referral rate is roughly 1 percent.
When and how will my baby be screened?
It is important to understand when and how your baby’s hearing screen will happen. It is recommended that a hearing screen be completed before discharge from a birthing facility or as soon after birth as possible for infants born at home. The Joint Committee on Infant Hearing advocates that all infants have their hearing screened by 1 month of age. If your newborn does not pass the first screen, some hearing screen providers will rescreen a baby before discharging the infant from the hospital. Our screeners test early to ensure the screen does not delay the discharge process.
Some screening programs will bring your baby elsewhere in the hospital to perform the screen. The Pediatrix Newborn Hearing Screen Program is mobile. Our screeners go where your baby is to perform the hearing screen, which is often at the bedside. However, if a medical reason causes your baby to be relocated within the hospital — such as the nursery or neonatal intensive care unit (NICU) — our technology can follow. You also don’t have to worry about when your baby is born. Our hearing screen professionals are available 365 days a year, seven days a week, including holidays. We are there when you and your baby need us.
The ideal conditions for a hearing screen involve screening in a quiet room when the infant is calm or sleeping. A baby must also pass the hearing screen in both ears. If any factors cause the infant to refer the test in one or both ears, the baby will be rescreened. It is possible for a newborn to not pass the first screen and still have normal hearing. Causes for not passing an initial hearing screen include:
- Vernix (waxy birthing substance) in the ear canal
- Fluid in the middle ear
- Movement and/or crying during the test
- Infant hearing loss
Rescreening may eliminate some of these factors. However, if an infant does not pass a rescreen, only diagnostic follow-up testing can reveal if it is due to the presence of hearing loss.
Does your hearing screen program use the most advanced screening technology?
There are two types of newborn hearing screens: Otoacoustic Emissions (OAE) and Automated Auditory Brainstem Response (A-ABR). Both are safe, approved by the Food and Drug Administration and comfortable for an infant; however, they differ in the thoroughness of their results. OAEs test a specific part of our hearing system only, the cochlea. The OAE screen does not test the functioning of the entire hearing system. For OAE testing, a small probe with a microphone is placed in the ear canal to collect a response from the cochlea. If the machine cannot detect a response with confidence, the infant will refer the hearing screen. A refer screening would result in the need for additional diagnostic testing.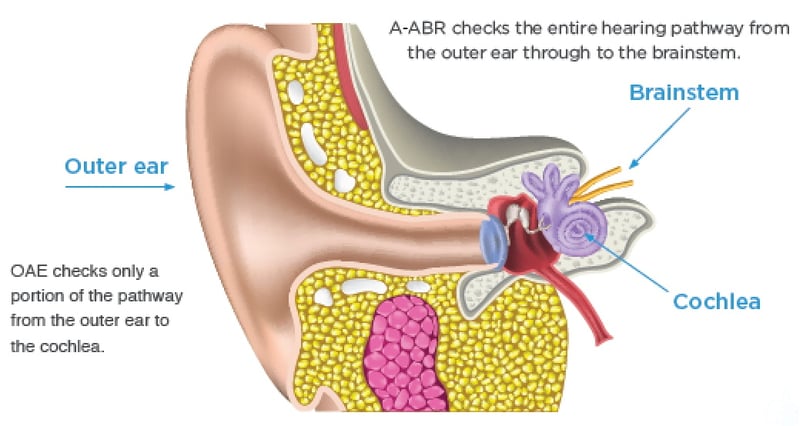 A-ABR screening tests both the cochlea and the hearing nerve — the complete hearing pathway, which carries sound to the brain. Some screening providers use the OAE test because it is less expensive, and rely on A-ABR screening if an infant refers the OAE screen. We believe A-ABR is a superior screening method because it tests both portions of the hearing pathway — the cochlea and the hearing nerve — to ensure the ears have adequate access to sound. Our screeners test all newborns with A-ABR technology only, not just infants in the NICU who may be at an increased risk for hearing loss. Regardless of the type of test used by a screening provider, for infants who do not pass the initial screen, follow-up testing is essential to help babies with infant hearing loss reach the final step of intervention
A-ABR screening tests both the cochlea and the hearing nerve — the complete hearing pathway, which carries sound to the brain. Some screening providers use the OAE test because it is less expensive, and rely on A-ABR screening if an infant refers the OAE screen. We believe A-ABR is a superior screening method because it tests both portions of the hearing pathway — the cochlea and the hearing nerve — to ensure the ears have adequate access to sound. Our screeners test all newborns with A-ABR technology only, not just infants in the NICU who may be at an increased risk for hearing loss. Regardless of the type of test used by a screening provider, for infants who do not pass the initial screen, follow-up testing is essential to help babies with infant hearing loss reach the final step of intervention
If my baby needs to see an audiologist, do you provide additional support?
Early identification of infants who need a more in-depth assessment of their hearing pathway is the first step in the hearing screen process. The Early Hearing Detection and Intervention (EHDI) guidelines include:
- Early Detection (before 1 month)
- Early Diagnosis (before 3 months)
- Early Intervention (before 6 months
These recommendations encourage a baby to be screened before turning 1 month old. If a baby does not pass the hearing screen, the EHDI protocol encourages follow-up testing to be completed before the infant reaches 3 months of age to better determine the absence or presence of hearing loss and accompanying level and type of hearing loss. Through early diagnosis, a baby with hearing loss can receive intervention before turning 6 months old.
Pediatrix supports the EHDI 1-3-6 goals and focuses on a team approach, working with audiologists, providers, primary care physicians and state and community resources, as well as families and hospital partners, to identify and assess babies at risk for hearing loss. If a baby needs to see an audiologist, our screening program helps to facilitate the follow-up appointment with reminders to families and reports to our provider and hospital partners. Our proprietary, web-based data management system helps our hearing screen program function more effectively by tracking your results and communicating with our provider and hospital partners to focus on that important step of assessment follow-up.
The American Speech-Language-Hearing Association is dedicated to “making effective communication, a human right, accessible and achievable for all.” Through Better Hearing & Speech Month, the national organization focuses on awareness of communication disorders. Pediatrix Newborn Hearing Screen Program is a proud partner in this effort, offering a national network with support at the state and local levels.
Learn more about Pediatrix Newborn Hearing Screen
.png)