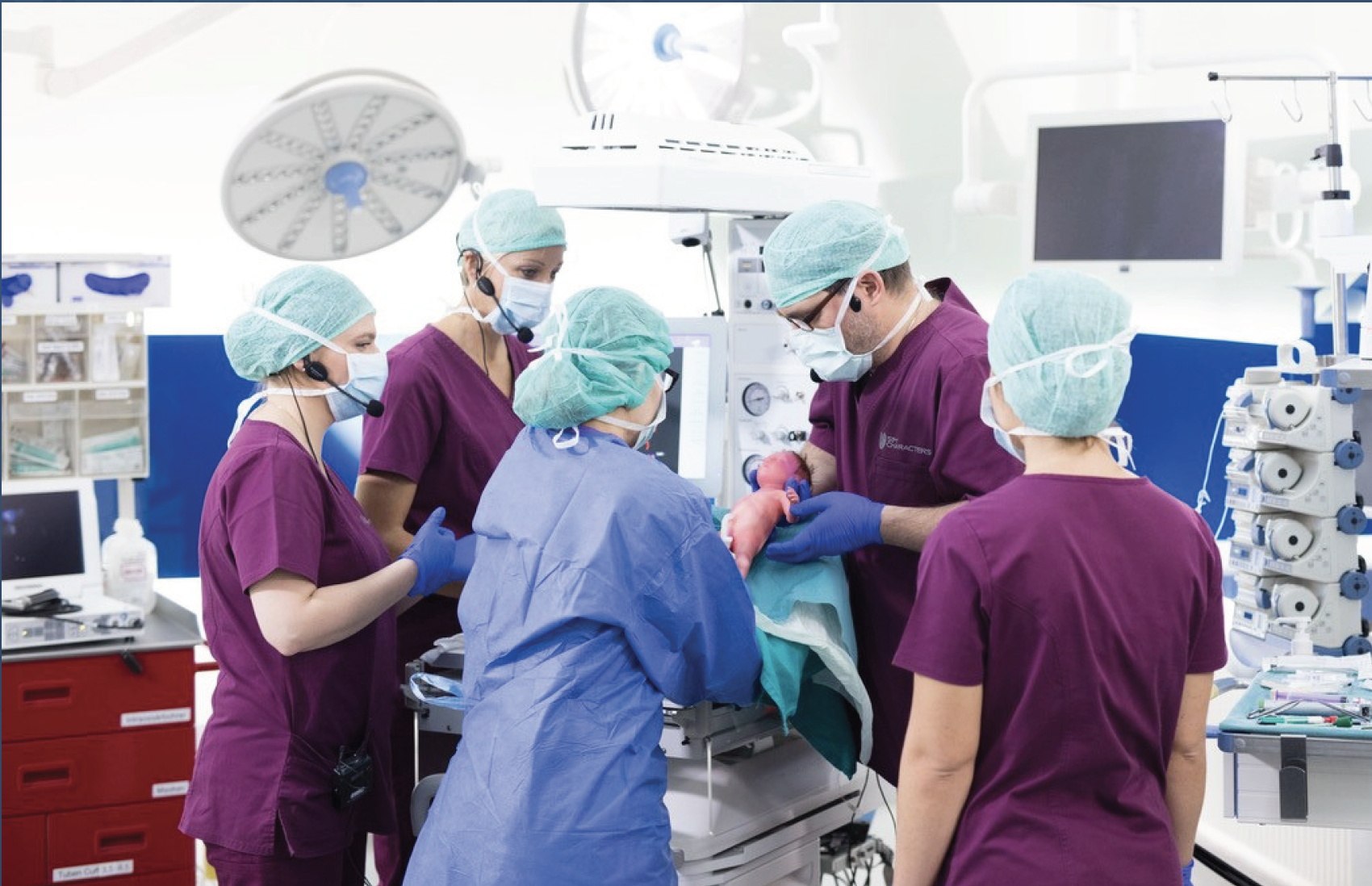
The MEDNAX simulation team presented two storyboards about their mobile national simulation program at the 2019 Institute for Healthcare Improvement Patient Safety Congress in Houston, TX, this May. The event draws attendees who treat patients in all types of environments, including hospitals, outpatient settings and home care.
“This annual meeting brings together people who are passionate about ensuring safe care equitably all across the globe to showcase the latest research, most innovative initiatives and emerging topics in patient safety,” said Diana Galvis, MBA, MEDNAX Senior Manager of HRO and Simulation. The storyboards presented by the MEDNAX simulation team provide a comprehensive look at developing a simulation program, including laying a program’s foundation and lessons of successful implementation.
Simulation serves to educate, assess, investigate and/or integrate best practices within a health care system or setting by safely replicating complex patient care scenarios without the negative effects of human or system error. This training serves to bridge the gap between the classroom and clinical experience, giving health care providers and hospitals a competitive edge when addressing a variety of high-stakes scenarios.
STORYBOARD 1
Building Your Own Simulation Program: A Blueprint for Success
 This presentation was developed by William Enfinger, DCE, CHSOS, Associate Director of Simulation Technology; Jaclyn LeVan, DO, MEDNAX-affiliated neonatologist; Julie Dyer, RN, NNPBC, MEDNAX-affiliated neonatal nurse practitioner; Gillian Gonzaba, RN, NNPBC, Associate Director of HRO and Simulation; Diana Galvis, MBA, Senior Manager of HRO and Simulation and Ingrid Vasiliu-Feltes, MD, MBA, Chief Quality and Innovation Officer. It outlines the fundamentals of the MEDNAX simulation program.
This presentation was developed by William Enfinger, DCE, CHSOS, Associate Director of Simulation Technology; Jaclyn LeVan, DO, MEDNAX-affiliated neonatologist; Julie Dyer, RN, NNPBC, MEDNAX-affiliated neonatal nurse practitioner; Gillian Gonzaba, RN, NNPBC, Associate Director of HRO and Simulation; Diana Galvis, MBA, Senior Manager of HRO and Simulation and Ingrid Vasiliu-Feltes, MD, MBA, Chief Quality and Innovation Officer. It outlines the fundamentals of the MEDNAX simulation program.
This program offers dynamic team training with a curriculum that involves a broad range of simulation scenarios focused on education, communication, patient safety and quality improvement. Implementation of the program includes:
- Interdisciplinary care team dynamics and TeamSTEPPS™ strategies
- Quality and safety measures specific to local practices
- Consultation to optimize or develop the use of simulation lab/equipment
- Train-the-trainer and standards implementation
- Feedback on team performance and potential areas for process improvement
To accommodate the simulation needs of our national network, the implementation of a mobile program was essential to provide in situ (“in place”) training, which allows providers to focus on building and assessing skills at their own facility without the distraction of an unfamiliar setting.
In an effort to enhance teamwork and communication, the simulation program incorporates:
- Just-in-time training
- Process improvement
- New-hire on-boarding
- Advancement in levels of care
- Error mitigation
- TeamSTEPPS™ implementation
High-fidelity and high-emotion manikins — including neonatal, newborn and mother/adult — are some of the assessment tools used during simulation training. The simulation scenarios draw from MEDNAX subject matter expertise in neonatology, pediatrics, obstetrics, maternal-fetal medicine and anesthesia, as well as simulation industry templates and development tools.
Each practice or facility undergoing simulation training is asked to develop objectives and use the SMART method to evaluate their goals and the ways in which simulations can help the team achieve its stated goals. The simulation process also includes facilitation and debriefing (with a focus on observation, evaluation, metrics and national standards and guidelines).
STORYBOARD 2
Lessons learned from launching a successful rapid-cycle deliberate practice (RCDP) program
 This presentation was developed by Gillian Gonzaba, RN, NNPBC; Jaclyn LeVan, DO; Julie Dyer, RN, NNPBC; William Enfinger, DCE CHSOS; Diana Galvis, MBA and Ingrid Vasiliu-Feltes, MD, MBA. It examines the benefits of rapid-cycle simulation training.
This presentation was developed by Gillian Gonzaba, RN, NNPBC; Jaclyn LeVan, DO; Julie Dyer, RN, NNPBC; William Enfinger, DCE CHSOS; Diana Galvis, MBA and Ingrid Vasiliu-Feltes, MD, MBA. It examines the benefits of rapid-cycle simulation training.
Unlike traditional simulation, where participants experience a simulation exercise with a debriefing following completion of the event, the MEDNAX simulation program employs rapid-cycle deliberate practice (RCDP). Through RCDP, teams experience rapid repetition of an event to achieve mastery. Research has shown RCDP can improve procedural proficiency and group dynamics within medical teams. First introduced in June 2018, the MEDNAX simulation team has seen a nearly 200 percent rise in utilization and RCDP requests.
The MEDNAX simulation scenarios are developed in collaboration with the local hospital to evaluate and assess the desired objectives. Critical stopping points are identified based on national standards and guidelines, including Neonatal Resuscitation Program®(NRP), American College of Obstetricians and Gynecologists (ACOG), California Maternal Quality Care Collaborative (CMQCC), Pediatric Advanced Life Support (PALS) and Advanced Cardiovascular Life Support (ACLS). Data is collated for each simulation exercise to provide key performance indicator feedback on time-to-intervention and any improvements made through the repetitive cycles. Patient safety strategies outlined by the Agency for Healthcare Research and Quality (AHRQ) through TeamSTEPPS are also assessed and evaluated so that hospitals may identify areas for quality improvement regarding leadership, communication and safety.

About the MEDNAX simulation program
MEDNAX simulation began with competency-based simulation and has since evolved to a focus on quality and patient safety. In 2017 and 2018, simulation gained traction in other service lines, leading to the development of unique, formalized programs. Beginning in 2019, the MEDNAX simulation program began consultative services and multisystem simulations.
The MEDNAX simulation program holds provisional accreditation by the Society for Simulation in Healthcare through December 2019. This is the first step required for full accreditation. MEDNAX simulation offers interactive programs for neonatology, anesthesiology and hospital-based medicine practices.
Have a question about our simulation program? Reach out